Maggots in Her Vagina: Causes, Symptoms, and Treatment Options
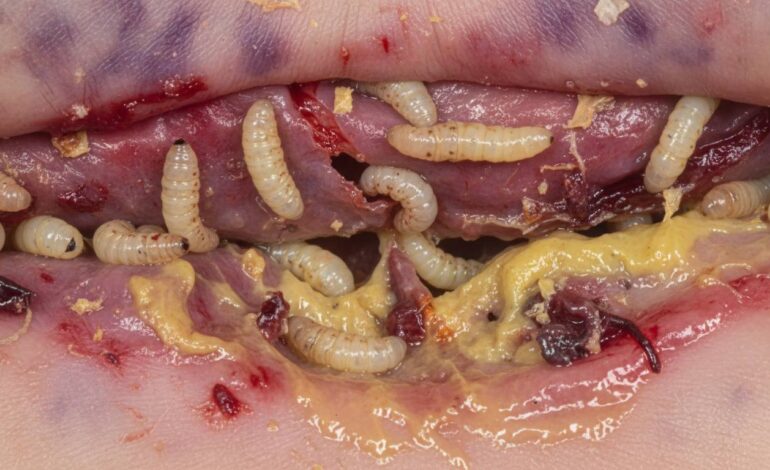
The presence of maggots in the vagina—medically referred to as vaginal myiasis—is a deeply distressing and rare condition. It happens when fly larvae infest living tissue, often linked to poor hygiene, untreated wounds, or living conditions conducive to flies. Immediate medical treatment, including removal of larvae, thorough cleaning, medication, and sometimes surgery, is essential to prevent complications and promote healing.
Understanding Vaginal Myiasis: What’s Going On?
Vaginal myiasis is astonishingly rare, yet undeniably serious. It happens when certain fly species deposit eggs in moist, decaying, or necrotic tissues near or inside the vagina. Over time, these hatch into larvae—or maggots—that feed on the tissue.
This scenario can sound more like a horror flick—real, almost unimaginable. It tends to happen where hygiene breaks down significantly or medical care is inaccessible. Even then, it remains exceptionally uncommon. Still, when it does occur, understanding the cause becomes instantly critical.
Why maggots, though?
Flies are drawn to damp, untreated, or infected tissue. In rare cases, this can include genital areas—particularly if there are menstrual complications, untreated injuries, or very poor sanitation. While uncommon in modern clinical settings, such infestations underscore the critical role of healthcare and cleanliness.
Causes: How It Happens
1. Poor Hygiene and Sanitation
Shocking as it sounds, neglected wounds or unhygienic environments can invite flies. In regions lacking clean water, sanitation, or private care, genital areas can become vulnerable.
2. Wounds or Necrotic Tissue
Untreated skin tears, lesions, or ulcerative changes around the vulva or vagina can become susceptible to infestation. Flies seek these out for egg-laying.
3. Menstrual Hygiene Issues
Improper disposal or prolonged use of sanitary products may create a breeding ground for flies—particularly in settings where replacement isn’t possible.
4. Immunocompromised State
Those with weakened immune systems may be more prone to infections or ulcers, raising vulnerability. Although your body fights off minor threats, maggot infestation is beyond that scope.
Symptoms: Recognizing the Red Flags
Knowing what to look for can be scary—but awareness saves lives. Main symptoms often include:
- Intense itching and a crawling sensation
- Visible worm-like movement
- Pain, swelling, or discharge—often foul-smelling
- Bleeding or ulceration in persistent cases
These are not subtle signs. They’re distress signals that demand attention. If you or someone you know feels like something is crawling or sees larvae, that’s an immediate call for help.
Diagnosis: What Doctors Do Right Away
In medical settings, diagnosis is usually swift. Here’s the usual process:
- Carefully inspect the affected area—often under good lighting or with assistance.
- Remove visible maggots with forceps or gentle irrigation.
- Take samples—both larvae and affected tissue—for lab identification.
- Evaluate for secondary infections or systemic spread.
Knowing it’s myiasis early can prevent complications like systemic infection or deeper tissue damage.
Treatment Approaches: What Really Works
Here’s how treatment typically unfolds:
1. Larvae Removal
Doctors start by physically removing all larvae. That can involve irrigation with antiseptics, gentle cleansing, or meticulously picking them out.
2. Cleansing and Debridement
If there’s dead or infected tissue, doctors remove it to help the area heal. That also reduces the chance of more infestation and gives the tissues a fighting chance.
3. Medication
Antibiotics are prescribed to control or prevent infections. In severe infestations, antiparasitic agents like ivermectin may be used—though that depends on the species and severity.
4. Wound Care & Hospitalization
Healing comes next: keeping the area clean, using antiseptic dressings, and close monitoring—sometimes even surgery in extreme cases.
5. Follow-Up
Just once isn’t enough. Regular check-ups help ensure healing and prevent recurrence.
Real-World Example: A Case Study
Picture a rural patient in a low-resource area. She noticed pain and discharge, dismissed it due to stigma. Over time, she felt something crawling. By the time she reached a clinic, maggots had taken root.
Local healthcare workers removed larvae gently, cleaned the area, and provided antibiotics. She recovered fully, but only because of timely intervention. It highlights how stigma or delays can turn a treatable condition into a dangerous one.
Preventing Vaginal Myiasis: Common Sense with Real Impact
Prevention is practical—still simple, but often overlooked:
- Maintain regular hygiene, especially around genital areas.
- Handle wounds properly—clean and protect them until healed.
- Use clean, breathable sanitary supplies and change them regularly.
- Seek medical help early if signs of infection appear.
These steps might seem basic, but they’re the difference between safety and nightmare.
“Even rare conditions like myiasis remind us of the importance of hygiene and access to basic healthcare,” says a rural health practitioner. “Addressing these can make all the difference.”
Why Understanding This Matters
This subject gets overlooked because it’s rare and uncomfortable to talk about. But awareness makes a difference—especially in areas lacking hygiene or medical care. It’s not just a medical topic—it’s a window into the broader issues of women’s health, stigma, and global disparity.
Conclusion
In short: maggots in the vagina are a rare but serious medical emergency. Infested tissue usually stems from poor hygiene, wounds, or healthcare delays. Symptoms are vivid and alarming, making early treatment vital. Medical care focuses on safe removal, cleaning, medications, and follow-up. And yes, avoiding it is all about basic health practices and access.
Hidden as it might be, this topic touches on bigger issues—women’s dignity, care equity, and our shared need for basic sanitation. Stay aware. Stay safe. Speak up if something’s off.
FAQs
What exactly causes maggots to infest genital tissue?
Flies are drawn to moist, damaged, or decaying tissue for egg-laying. In rare cases—especially with poor hygiene or untreated wounds—larvae can develop in genital areas.
How would someone know if they might have this?
Visual cues like crawling movement, intense itching, swelling, or foul discharge are key signs. Itchy or painful symptoms shouldn’t be ignored.
What happens during medical treatment for this condition?
Doctors will remove larvae manually, clean or debride affected tissue, prescribe antibiotics or antiparasitics if needed, and monitor healing until recovery.
Can this happen in developed countries?
It’s extremely rare in places with robust healthcare or sanitation. But it can still occur in neglected wounds or severe hygiene lapses. Awareness matters everywhere.
Is this condition life-threatening?
It can become serious if untreated—leading to infections or deeper tissue damage. With early medical care, though, recovery is highly likely.
How can I reduce my risk of something like this?
Keeping genital and menstrual hygiene good, tending to wounds, and seeking prompt medical help for any concerning symptoms are your best protection.